Reports of research work funded by grants prior to 2016
University of Otago Wellington
Premature birth and the pancreas: the impact of preterm birth on adult metabolic dysfunction
M Berry
Department of Paediatrics and Child Health
The specific aims of this grant were to:
- To use our novel preterm guinea pig paradigm to test the impact of premature birth and early nutritional environment on later metabolic function.
- To consolidate a Wellington-based collaboration of expertise in Neonatology, Endocrinology and Translational Biomedical Research.
The funding provided through WMRF has enabled significant progress to be made in our understanding of how preterm birth continues to influence metabolic health beyond the neonatal period. We would like to highlight however that the time taken to generate preterm animals and follow their metabolic health over time means that this report reflects only a small proportion of the work that is currently underway. Additionally, the detailed metabolic pathway analyses being undertaken on this cohort required development of new methodologies. The latency that inevitably results from these sorts of animal studies means that many of the final results and data analysis are yet to come.
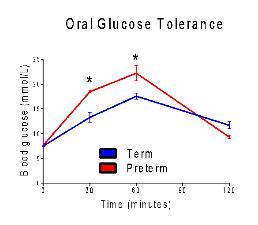
One of the main outcomes of this study was to assess the impact of preterm birth on glucose tolerance. We have demonstrated the juvenile animals born preterm are glucose intolerant compared to those born at full term. This demonstrates that the animals capacity to clear glucose efficiently from their system is impaired, a possible pre-cursor to the development of diabetes.
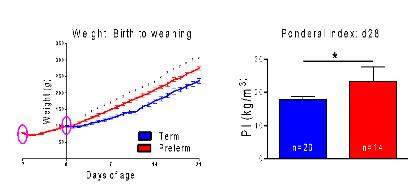
We have also confirmed our preliminary results and demonstrated altered patterns of growth and increased adiposity (ponderal index; a measure of relative weight for length) in pre-pubertal animals born preterm.
Humans born preterm have a greater risk of developing an unhealthy pattern of fat distribution and diabetes or impaired glucose metabolism in adult life than individual born at full term. The parallels between the human condition and our animal model mean that lessons learned from the guinea pig model will be of great value in assisting clinicians to understand the mechanistic pathways linking early life environment with later outcomes. Additionally, it is plausible that diabetic risk due to preterm birth is regulated differently than diabetic risk due to sedentary lifestyle or other environmental factors in adulthood. By understanding the way in which this increased metabolic risk (impaired glucose tolerance and altered fat distribution) is regulated, we may be able to develop novel therapeutic interventions targeting the unique health needs of those already disadvantaged by premature birth. Detailed analysis of the gene expression and enzyme pathways in liver, muscle and fat that play a major role in glucose and fat metabolism are under investigation by our collaborators.
This project has additionally been instrumental in strengthening the collaborative links between our team of Wellington-based academics (University of Otago, Wellington and ESR) and our colleagues at the University of South Australia, the University of Adelaide and elsewhere. These linkages will enable us to significantly increase the productivity and outputs from the novel animal model of preterm birth developed here in Wellington by allowing us to access state-of-the-art laboratory techniques not currently available locally.
Data from these studies were presented this year at invited Plenary sessions at the Perinatal Society of Australia and New Zealand annual conference and at the Developmental Origins of Health and Disease ANZ annual conference. The resultant manuscripts are in preparation and should be submitted within the next six months.
Due to logistical issues beyond our control, we have been unable to test the impact of imposing a preterm feeding regimen onto term-born animals. However, this does not detract from the impact of the work that has been completed and its implications for the better understanding of lifelong health and disease risk following preterm birth.



